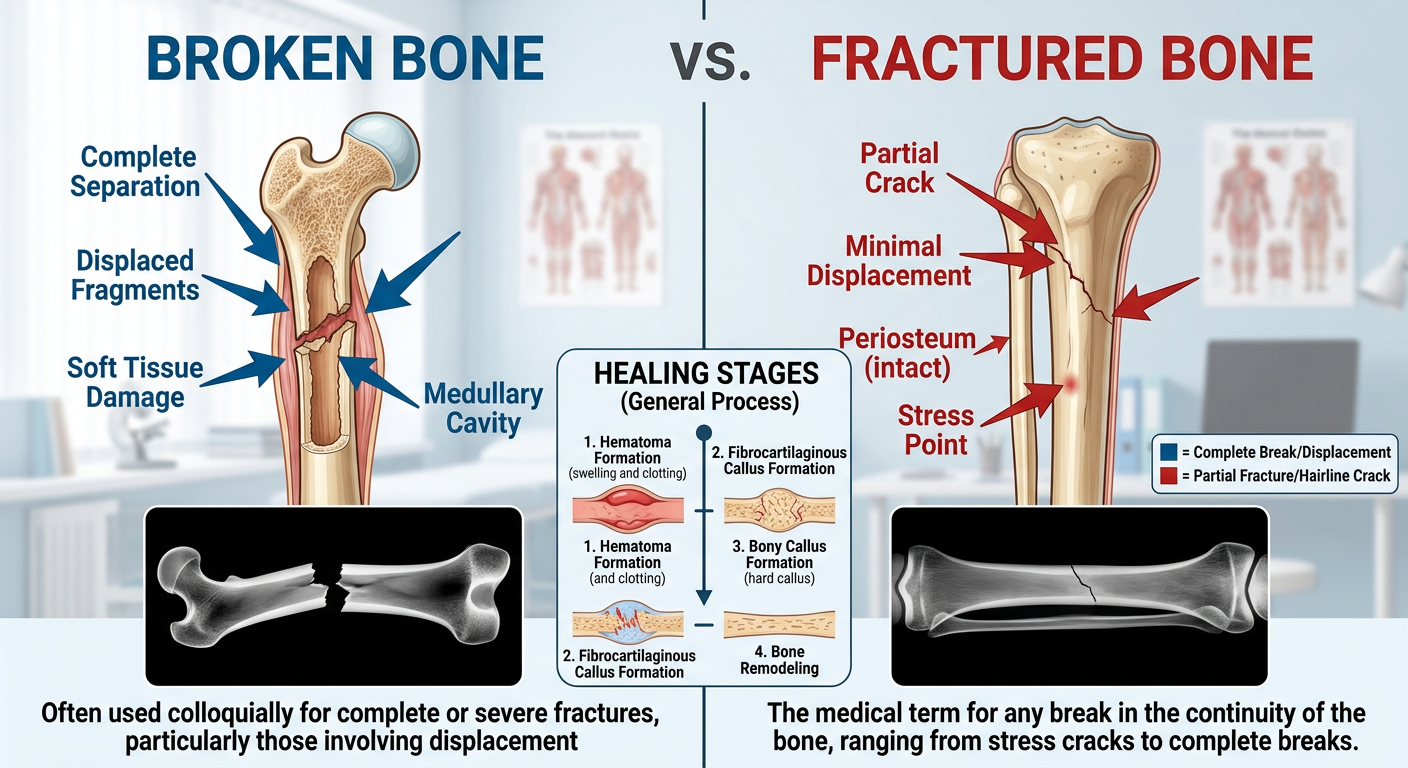
You’ve probably heard someone say, “I broke my arm,” while a doctor writes “fracture” on the medical report. This common scenario leaves many people wondering: are they talking about different injuries?
Many people believe a fracture is somehow less serious than a broken bone. Some even think a fracture means the bone is cracked but still intact, while a break means it has snapped completely in two. This is one of the most widespread misconceptions in everyday medical understanding.
The truth might surprise you.
In medicine, a broken bone and a fracture are exactly the same thing. Doctors use both terms to describe any disruption in bone continuity, from a hairline crack to a bone shattered into multiple pieces.
In this article, you’ll learn what fractures really mean, the many types that exist, how they’re diagnosed and treated, and how long recovery takes. Whether you’ve just experienced an injury or simply want to understand bone health better, this complete guide covers everything you need to know.
Understanding the correct terminology helps you communicate more effectively with healthcare providers and make informed decisions about your treatment.
Understanding the Terminology
What Is a Fracture?
The medical definition of a fracture is any break in the continuity of a bone. This definition is intentionally broad. It includes everything from a tiny stress crack that barely shows on an X-ray to a severe injury where bone fragments pierce through the skin.
The word “fracture” comes from the Latin word fractura, meaning “a break.” Interestingly, the Latin root frangere means “to break.” So even the word itself confirms that a fracture is, by definition, a break.
From a clinical standpoint, a fracture occurs when a force applied to a bone exceeds the bone’s structural strength. This can happen suddenly through trauma or gradually through repeated stress. Either way, the result is classified as a fracture.
Orthopedic surgeons, emergency physicians, and radiologists all use the term “fracture” in their official documentation. You will rarely see the term “broken bone” in a medical chart, though both descriptions refer to the same condition.
What Does “Broken Bone” Mean?
“Broken bone” is the everyday, non-medical way of describing a fracture. It’s the term most people grew up using and the one they instinctively reach for when explaining an injury to friends and family.
From a medical perspective, “broken bone” is accurate, just informal. There is no clinical distinction between a broken bone and a fracture. Doctors themselves often use “broken bone” in patient conversations because it’s easier for most people to understand.
The term persists because it creates a clear mental image. When you hear “broken bone,” you immediately understand that something serious has happened. It communicates urgency and severity in a way that resonates with everyday experience.
The Simple Answer: Are They the Same?
Yes, completely and without exception.
Every fracture is a broken bone, and every broken bone is a fracture. There is no medical scenario where one term applies and the other does not. The American Academy of Orthopedic Surgeons, the Mayo Clinic, and every major medical institution confirm this.
The confusion exists for a few reasons. First, “fracture” sounds technical and partial, while “break” sounds total and devastating. Second, common phrases like “it’s just a hairline fracture” lead people to believe some fractures aren’t real breaks. Third, television and movies often dramatize the difference, reinforcing the misconception.
The reality is simple: if your bone is fractured, it is broken. Period.
Types of Fractures Explained
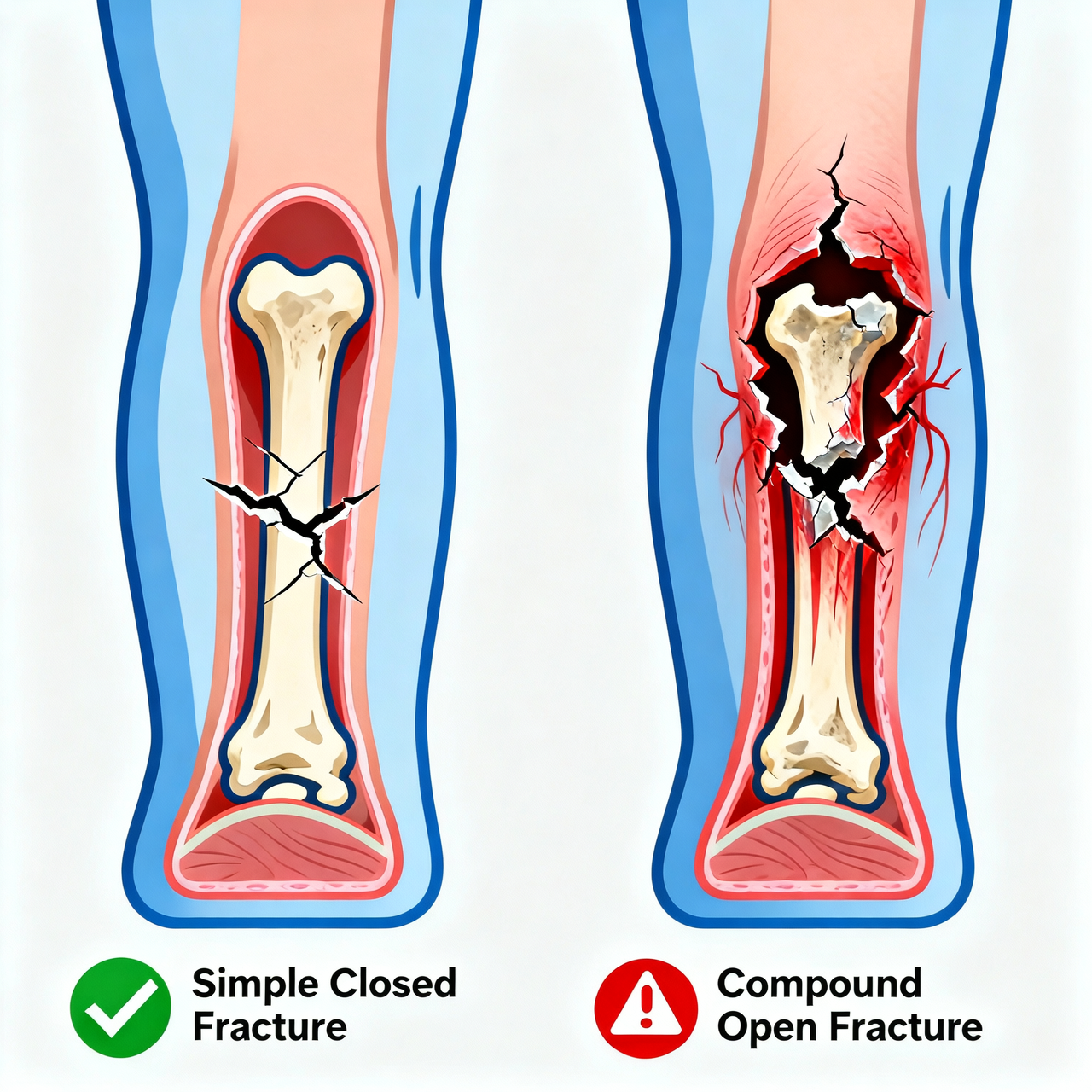
Not all fractures are created equal. Doctors classify them based on the pattern of the break, the severity, and whether surrounding tissues are affected. Understanding the different types helps explain why some fractures heal quickly with a simple cast while others require complex surgery.
A. Simple (Closed) Fractures
A simple fracture, also called a closed fracture, occurs when the bone breaks but does not pierce through the skin. The surrounding skin and soft tissue remain intact.
These fractures are generally less severe than open fractures because the risk of infection is significantly lower. However, “simple” does not mean painless or minor. A closed fracture can still cause significant swelling, bruising, and prolonged recovery.
Common causes include:
- Trips and falls
- Sports collisions
- Direct impact to a limb
A broken wrist from catching yourself during a fall is a classic example of a simple closed fracture.
B. Compound (Open) Fractures
A compound fracture, or open fracture, is far more serious. In this type, the broken bone pierces through the skin and becomes exposed to the outside environment.
This exposure creates an immediate and serious infection risk. Bacteria can enter the wound and reach the bone, potentially causing osteomyelitis, a deep bone infection that is notoriously difficult to treat.
Open fractures almost always require emergency surgery. Surgeons must clean the wound thoroughly, realign the bone, and stabilize it. Intravenous antibiotics are typically administered immediately.
These injuries commonly result from high-speed car accidents, motorcycle crashes, or severe falls from significant heights.
C. Hairline (Stress) Fractures
Hairline fractures are microscopic cracks in bone that develop gradually rather than from a single traumatic event. They are also called stress fractures because they result from repetitive stress applied to the bone over time.
Athletes are particularly vulnerable, especially runners, gymnasts, and basketball players. When muscles fatigue, they transfer more impact force to the underlying bone. Over time, this repeated stress creates tiny cracks.
Symptoms often include:
- Dull aching pain that worsens with activity
- Tenderness to the touch over a specific area
- Mild swelling
Diagnosis can be tricky because hairline fractures may not appear on standard X-rays for several weeks. MRI scans are often more reliable for early detection.
D. Greenstick Fractures
Greenstick fractures occur almost exclusively in children. In this type, the bone bends and partially breaks on one side but remains intact on the other, much like a young, green tree branch that bends and splits rather than snapping cleanly.
Children’s bones are still developing and contain more collagen, making them more flexible than adult bones. This flexibility is generally protective but also creates this unique fracture pattern.
The healing process for greenstick fractures is typically faster than for adult fractures because children’s bones have a superior blood supply and higher metabolic activity. Most children recover well with casting alone.
E. Comminuted Fractures
Comminuted fractures involve the bone shattering into three or more fragments. These are among the most complex fractures to treat.
They typically result from high-energy trauma such as:
- Severe motor vehicle accidents
- Falls from significant heights
- High-velocity gunshot wounds
Surgical treatment is almost always required. Surgeons use metal plates, screws, and rods to reassemble the bone fragments as precisely as possible. Recovery is lengthy, and outcomes depend heavily on the location and extent of fragmentation.
F. Compression Fractures
Compression fractures occur when a vertebra in the spine collapses or is crushed. They are strongly associated with osteoporosis, a condition that causes bones to become brittle and porous.
In severe osteoporosis, a compression fracture can occur with minimal force, sometimes from simply bending forward or sneezing. The elderly are at particularly high risk.
Warning signs include:
- Sudden onset of back pain
- Gradual loss of height over time
- A stooped or hunched posture
Treatment ranges from rest and pain management to minimally invasive procedures like vertebroplasty or kyphoplasty, where bone cement is injected to stabilize the collapsed vertebra.
G. Other Types
Several additional fracture patterns are worth understanding:
- Oblique fractures: The break runs at a diagonal angle across the bone, often caused by a twisting force combined with impact
- Transverse fractures: The break runs straight across the bone in a horizontal line, typically from a direct blow
- Spiral fractures: The fracture spirals around the bone’s shaft, classically caused by a rotational or twisting force
- Avulsion fractures: A fragment of bone is pulled away by a tendon or ligament during a sudden, forceful movement, common in ankle injuries and sports
Common Causes of Bone Fractures
A. Traumatic Injuries
Traumatic injuries are the most recognizable cause of fractures. They involve a sudden, forceful event that overwhelms the bone’s structural strength.
Common traumatic causes include:
- Falls: The leading cause of fractures, especially in children and the elderly
- Car accidents: High-impact collisions frequently cause fractures of the legs, pelvis, ribs, and spine
- Sports injuries: Contact sports, skiing, and cycling all carry significant fracture risk
- Direct blows: A hard impact from a blunt object can break bones at the point of contact
B. Overuse and Repetitive Stress
Not all fractures happen in a single moment. Repetitive loading of a bone can cause it to fail gradually.
Runners who dramatically increase their weekly mileage, military recruits in basic training, and dancers who practice for hours daily are all at elevated risk for stress fractures. The second metatarsal bone in the foot is among the most commonly affected sites.
Occupational hazards also contribute. Workers who perform repetitive physical tasks without adequate rest periods can develop stress fractures in weight-bearing bones.
C. Medical Conditions
Several underlying health conditions weaken bones and make fractures more likely:
- Osteoporosis: Reduces bone density and dramatically increases fracture risk
- Cancer: Both primary bone cancer and cancer that spreads to bone can destroy structural integrity
- Osteogenesis imperfecta: A genetic disorder sometimes called “brittle bone disease” that causes frequent fractures with minimal trauma
- Hyperparathyroidism: Excess parathyroid hormone draws calcium from bones, weakening them over time
D. Age-Related Factors
Age affects both fracture risk and the types of fractures that commonly occur. Children’s bones are flexible and resilient, but also growing rapidly, making them susceptible to unique fracture patterns like greenstick fractures.
The elderly face the opposite challenge. Bone density naturally declines after age 30 and accelerates after menopause in women. Reduced bone density combined with balance problems and medication side effects makes hip and spine fractures dangerously common in older adults.
Signs and Symptoms
A. Immediate Symptoms
When a bone fractures, the body responds immediately and dramatically. Recognizing these signs can help you seek the right care quickly.
Immediate symptoms include:
- Severe pain: Often described as sharp and intense, immediately following the injury
- Swelling: Develops rapidly as the body sends blood and fluid to the injured area
- Bruising: May appear within minutes or take several hours to become visible
- Deformity: The limb may appear bent, shortened, or angulated in an unnatural direction
- Inability to bear weight: Standing or walking becomes impossible with lower-limb fractures
- Audible sound: Many people describe hearing or feeling a distinct snap or crack at the moment of injury
B. Delayed Symptoms
Some symptoms develop hours or days after the initial injury:
- Prolonged pain that doesn’t improve with rest
- Increasing stiffness and limited range of motion
- Numbness or tingling, which can indicate nerve involvement
- Persistent swelling that doesn’t respond to elevation or ice
Stress fractures in particular may produce only mild, nagging pain initially, which gradually worsens with continued activity.
C. When to Seek Emergency Care
Call emergency services or go directly to an emergency room if you observe any of the following:
- Bone protruding through the skin
- Severe deformity of the affected limb
- Loss of sensation or circulation below the injury
- Signs of heavy bleeding that cannot be controlled
- Suspected fractures of the spine, pelvis, or femur
- Significant head or neck trauma accompanying the injury
Delaying care for these injuries can result in life-threatening complications, including severe blood loss or permanent nerve damage.
Diagnosis Methods
A. Physical Examination
A doctor’s first step is a careful physical examination. They will assess the location and severity of pain by applying gentle pressure. They will also evaluate circulation, sensation, and movement below the suspected fracture.
The physical exam helps doctors prioritize which imaging tests are needed and determine whether emergency intervention is required before results are available.
B. Imaging Tests
Imaging confirms the diagnosis and reveals the exact nature and location of the fracture.
| Imaging Type | Best Used For | Notes |
|---|---|---|
| X-ray | Most fractures | Fast, widely available, first-line test |
| CT Scan | Complex fractures, spine | Provides detailed 3D views of bone |
| MRI | Stress fractures, soft tissue | Best for detecting early or hidden fractures |
| Bone Scan | Stress fractures, cancer | Detects metabolic activity in bone |
X-rays remain the most commonly used diagnostic tool because they are quick, affordable, and effective for the majority of fractures. However, hairline fractures and stress fractures may not appear on X-rays for several weeks after the injury.
C. Additional Tests
When a medical condition may have contributed to the fracture, doctors may order:
- Blood tests: To evaluate calcium levels, vitamin D levels, or markers of bone disease
- Bone density testing (DEXA scan): To assess osteoporosis risk, particularly in postmenopausal women and older men
Treatment Options
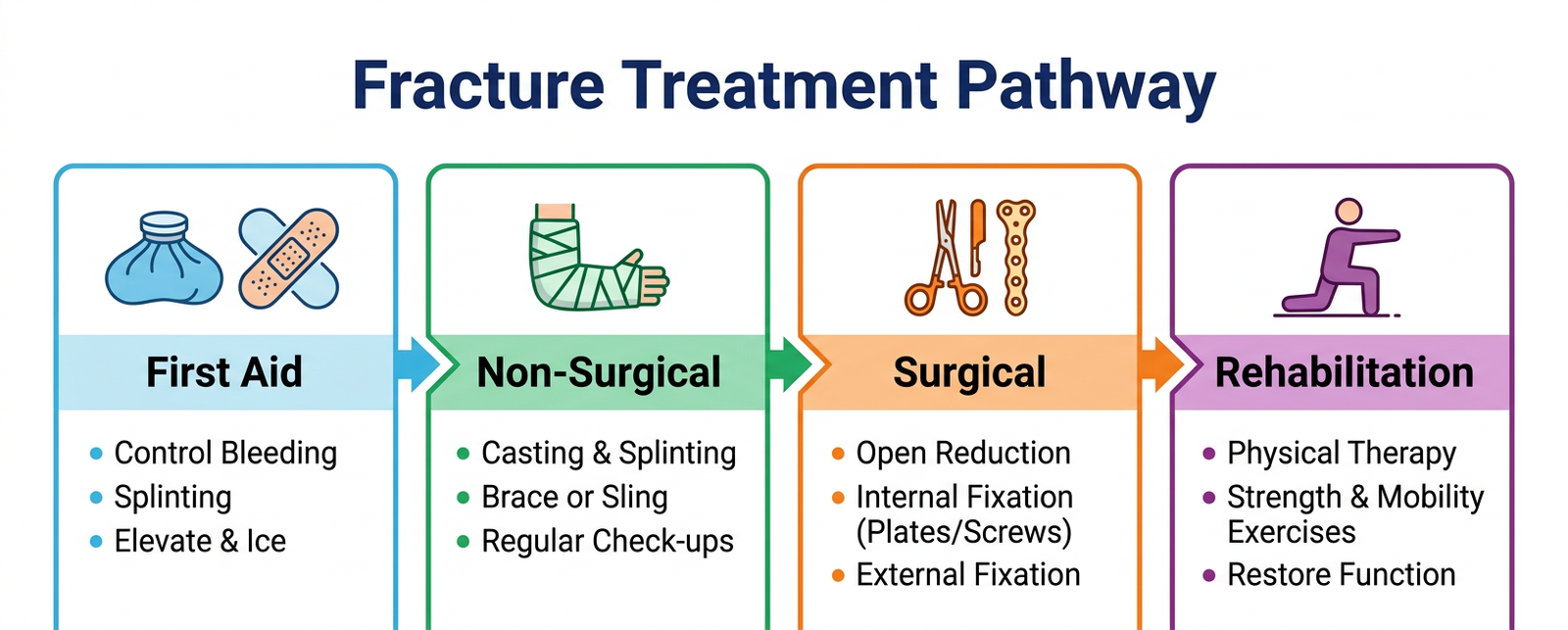
A. First Aid and Immediate Care
Before professional medical care is available, appropriate first aid can prevent the injury from worsening.
The R.I.C.E. method applies to suspected fractures:
- Rest: Stop all activity and avoid putting weight on the injured area
- Ice: Apply ice wrapped in a cloth for 20 minutes at a time to reduce swelling
- Compression: A bandage can provide mild support, but avoid wrapping too tightly
- Elevation: Raise the injured limb above heart level when possible
Do NOT:
- Attempt to realign or straighten the bone yourself
- Remove clothing from around an open fracture wound
- Give food or water if surgery may be needed
- Allow the injured person to walk on a suspected lower-limb fracture
Immobilize the injury using a makeshift splint if transport is necessary. Rolled magazines, sticks, or folded blankets secured with strips of cloth can stabilize a limb effectively.
B. Non-Surgical Treatments
Many fractures heal successfully without surgery.
Casting and splinting remain the cornerstone of non-surgical fracture treatment. Casts hold the bone in proper alignment while it heals, typically over six to eight weeks for most arm and leg fractures.
Bracing is sometimes used for less severe fractures or during the later stages of recovery. Functional braces allow some controlled movement, which can actually promote healing in certain injury types.
Physical therapy typically begins after the cast or brace is removed. A structured rehabilitation program restores strength, flexibility, and range of motion that are lost during immobilization.
C. Surgical Interventions
Surgery is necessary when:
- The fracture is displaced and cannot be aligned by other means
- The fracture is open (compound)
- Multiple bone fragments are present
- The fracture involves a joint surface
Surgical options include:
- Internal fixation: Metal plates, screws, or intramedullary rods are inserted to hold bone fragments in proper alignment during healing
- External fixation: A metal frame is attached outside the body, connected to pins inserted through the skin into the bone, used when internal fixation isn’t immediately possible
- Bone grafting: Bone material from another part of the body or from a donor is used to fill gaps and stimulate healing in complex fractures
Recovery from surgical fixation is typically longer than non-surgical treatment, often ranging from several months to over a year for complex injuries.
D. Pain Management
Fracture pain can range from moderate to severe and must be managed effectively to support recovery.
Options include:
- Over-the-counter medications: Acetaminophen and ibuprofen for mild to moderate pain
- Prescription pain relievers: Short-term opioids may be appropriate for severe fractures in the immediate post-injury period
- Alternative therapies: Transcutaneous electrical nerve stimulation (TENS), acupuncture, and guided imagery can supplement medical pain management
Patients should discuss all pain management options with their healthcare provider, particularly regarding the appropriate duration of any prescription medication use.
Healing Process and Recovery Time
A. Stages of Bone Healing
Bone healing is a remarkable biological process that occurs in three overlapping phases:
- Inflammation phase (Days 1-7): Blood vessels at the fracture site rupture, forming a blood clot called a fracture hematoma. Immune cells arrive to clean up damaged tissue, and a temporary repair structure begins to form.
- Bone production phase (Weeks 2-8): Specialized cells called osteoblasts begin building new bone tissue. A soft callus forms around the fracture, gradually hardening into a bony callus that bridges the two bone ends.
- Bone remodeling phase (Months to years): The body refines the newly formed bone, reshaping it to restore normal structure and strength. Remarkably, healed bone can sometimes become stronger than the original bone at the fracture site.
B. Average Recovery Times
Recovery time varies considerably depending on which bone is fractured and how severely.
| Fracture Location | Approximate Healing Time |
|---|---|
| Finger | 3–5 weeks |
| Wrist | 6–8 weeks |
| Ankle | 6–8 weeks |
| Tibia (shin) | 4–6 months |
| Femur (thigh) | 4–6 months |
| Hip | 6–12 months |
| Vertebra | 6–12 weeks (mild compression) |
Children typically heal faster than adults. Elderly individuals often require significantly longer recovery periods.
C. Factors Affecting Healing
Several factors influence how quickly and completely a fracture heals:
- Nutrition: Adequate calcium, vitamin D, and protein are essential for bone formation. Deficiencies can delay healing significantly
- Smoking: Nicotine restricts blood flow and interferes with calcium absorption, slowing healing by up to 40% in some studies
- Alcohol: Heavy alcohol consumption impairs bone cell function and reduces bone density
- Underlying health conditions: Diabetes, kidney disease, and osteoporosis all negatively affect healing
- Compliance with treatment: Following medical advice about immobilization and activity restrictions directly impacts outcomes
Complications and Risks
A. Short-Term Complications
Even with proper treatment, certain complications can develop in the early stages of recovery:
- Compartment syndrome: Swelling within a closed muscle compartment cuts off blood supply, causing intense pain and potential tissue death. This is a surgical emergency
- Infection: Primarily a risk with open fractures or after surgical intervention
- Blood clots (deep vein thrombosis): Immobility after lower-limb fractures significantly increases the risk of clotting. Clots can travel to the lungs, causing a life-threatening pulmonary embolism
- Nerve damage: Bone fragments or severe swelling can damage nearby nerves, causing weakness or numbness
B. Long-Term Complications
Long-term complications can affect function and quality of life significantly:
- Delayed union or nonunion: The bone heals more slowly than expected or fails to heal entirely
- Malunion: The bone heals in an incorrect position, potentially causing deformity, pain, or limited function
- Post-traumatic arthritis: Fractures that involve joint surfaces frequently lead to arthritis developing in that joint over time
- Chronic pain: Some patients experience ongoing pain even after the bone has fully healed
- Osteomyelitis: Bone infection, particularly after open fractures, can become chronic and difficult to eradicate
Prevention Strategies
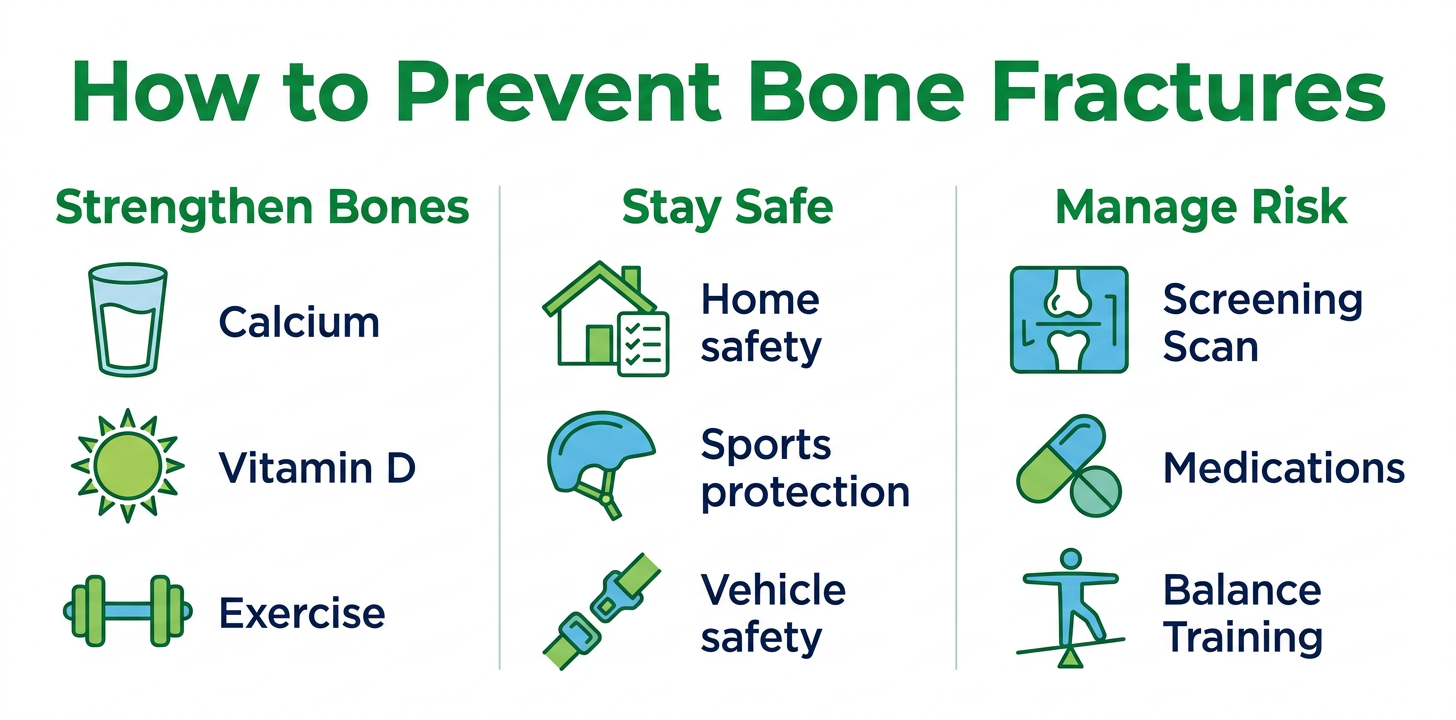
A. Strengthening Bones
Building and maintaining strong bones is the single most effective strategy for reducing fracture risk throughout life.
Key approaches include:
- Calcium intake: Adults need 1,000–1,200 mg of calcium daily. Good sources include dairy products, leafy greens, almonds, and fortified foods
- Vitamin D: Essential for calcium absorption. Aim for 600–800 IU daily through sunlight exposure, fatty fish, egg yolks, or supplements
- Weight-bearing exercise: Walking, jogging, dancing, and resistance training stimulate bone formation. Aim for at least 150 minutes of moderate activity per week
- Bone density screening: Women over 65 and men over 70 should have routine DEXA scans. Earlier screening is recommended for those with risk factors
B. Safety Measures
Preventing the accidents that cause fractures is equally important.
Home safety for fall prevention:
- Remove loose rugs and clutter from walkways
- Install grab bars in bathrooms and shower areas
- Ensure adequate lighting throughout the home
- Wear appropriate footwear with non-slip soles
Sports and workplace safety:
- Always wear appropriate protective equipment including helmets, wrist guards, and knee pads
- Increase training intensity gradually rather than dramatically
- Follow proper lifting techniques in occupational settings
- Use seatbelts and appropriate car seats in all vehicles
C. Managing Risk Factors
Addressing known risk factors significantly reduces fracture probability:
- Treating osteoporosis with appropriate medications, including bisphosphonates, when recommended by a physician
- Reviewing medications that may cause dizziness or affect balance, particularly in elderly patients
- Balance and coordination training: Tai chi and similar practices have demonstrated effectiveness in reducing fall risk in older adults
Frequently Asked Questions
Can you walk on a fractured bone?
It depends entirely on the fracture’s location and severity. Some people walk on fractured foot bones for days before seeking care because the pain is manageable. However, walking on a fractured weight-bearing bone can worsen the injury, displace the fracture, and cause additional damage to surrounding tissue. If you suspect a fracture in any lower-limb bone, avoid bearing weight and seek medical evaluation promptly.
How do you know if a bone is broken or just bruised?
This is genuinely difficult to determine without imaging. Bone bruises, which occur when the bone’s inner structure is damaged without a complete fracture, can be extremely painful and mimic fracture symptoms. Significant pain directly over a bone, rapid-onset swelling, and difficulty using the affected area are all reasons to get an X-ray. When in doubt, always have a medical professional evaluate the injury.
Do all fractures require a cast?
No. Treatment depends on the location, type, and severity of the fracture. Some small bone fractures, such as certain rib or toe fractures, are treated with rest and pain management alone. Others may require a splint, brace, or specialized boot rather than a traditional plaster cast. Your doctor will recommend the most appropriate immobilization method for your specific injury.
Can a fracture heal on its own?
Minor fractures in certain bones can heal with rest alone if the bone ends remain properly aligned. However, “healing on its own” without medical evaluation carries significant risks. A fracture that heals in a misaligned position can result in permanent deformity, chronic pain, and loss of function. Always have a suspected fracture evaluated by a medical professional, even if the pain seems manageable.
What’s worse: a break or a fracture?
They are identical. As established throughout this article, a break and a fracture are the same injury described with different words. Severity is determined by the type, location, and extent of the fracture, not by which term is used to describe it.
How long does a fracture take to heal?
Healing time ranges from three weeks for a minor finger fracture to a year or more for complex hip or femur fractures. The location of the fracture, your age, overall health, nutrition, and compliance with treatment all play significant roles. Your orthopedic specialist can give you the most accurate timeline for your specific injury.
Can you still move a broken bone?
Some movement is occasionally possible after a fracture, particularly with small bone breaks or stress fractures. This is one reason fractures are sometimes dismissed or ignored initially. The ability to move a body part does not rule out a fracture. Attempting to move a fractured limb can worsen the injury and cause additional pain, soft tissue damage, or displacement of bone fragments.
Do fractures show up on X-rays immediately?
Most fractures are visible on X-rays taken immediately after the injury. However, hairline and stress fractures may not appear on standard X-rays for two to three weeks, when healing bone formation becomes visible. If your X-ray is negative but you have persistent localized pain and a history consistent with a stress fracture, your doctor may order an MRI, which can detect these injuries within days of their occurrence.
Conclusion
The central answer to the question this article set out to address is clear: a broken bone and a fracture are one and the same. These terms are used interchangeably by medical professionals and patients alike to describe any disruption in bone continuity, regardless of severity.
Understanding this eliminates a common misconception that can delay appropriate care. Whether someone tells you they have “just a fracture” or a “broken bone,” the injury deserves prompt medical evaluation.
Bone injuries span a wide spectrum, from minor stress fractures that heal with rest to complex comminuted fractures requiring multiple surgeries and months of rehabilitation. Proper diagnosis through imaging, appropriate treatment, and adherence to medical guidance are all essential for the best possible outcome.
Most importantly, don’t attempt to self-diagnose or dismiss bone pain after trauma or repetitive stress. Seeking a professional evaluation promptly leads to a more accurate diagnosis, more appropriate treatment, and ultimately better recovery.
Take care of your bones through nutrition, exercise, and safety awareness. They are the framework that keeps you moving through every stage of life.
This article is intended for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis and treatment of any injury or medical condition.